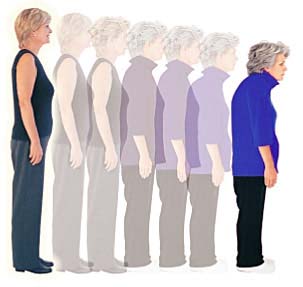
Reducing the risk of brittle bone disease
What is it and how does it happen?
Brittle bone disease (osteoporosis or ‘OP’) is a condition that most people tend to think of as a women’s illness simply because it’s so often associated with the menopause. It affects men too, albeit less commonly – although, some might jest, so does the menopause itself!
Put simply, osteoporosis occurs because, as we age, bones begin to lose calcium, causing porosity and increasing the risk of fractures. In the female of the species, the menopause and post-menopause are critical because the production of oestrogen (estrogen in the U.S.), the hormone that helps to lay calcium into the bones, first begins to dwindle and then eventually is no longer being produced by the ovaries. But some experts believe that thinning bones may have less to do with the menopause than with lifestyle and dietary habits and that there are steps we can all take to reduce the risk of osteoporosis.
Put simply, osteoporosis occurs because, as we age, bones begin to lose calcium, causing porosity and increasing the risk of fractures. In the female of the species, the menopause and post-menopause are critical because the production of oestrogen (estrogen in the U.S.), the hormone that helps to lay calcium into the bones, first begins to dwindle and then eventually is no longer being produced by the ovaries. But some experts believe that thinning bones may have less to do with the menopause than with lifestyle and dietary habits and that there are steps we can all take to reduce the risk of osteoporosis.
The figures
Everyone loses some bone density as the years advance but it’s estimated that approximately 33% of all women are potentially at risk from OP. One in every four over the age of sixty and half of those over seventy are likely to be affected. Around 100,000 fractures of hips and spines occur every year and more women die from complications following fractures than from major female cancers! Scary huh?
Osteoporosis is sometimes known as the silent disease because it may be present in the body for a long time without us noticing any symptoms. And as far as those symptoms are concerned, there may be some back pain, the odd muscle spasm or a slight curving of the spine or nothing at all until someone slips or trips. By the time thinning bones show up on an ordinary X-ray, as much as 30 percent of bone mass could already have been lost. That's why the recommended test is a bone density scan - usually done on the hip and the spine - which shows, as the name suggests, the existing density of those areas. However, bear in mind that scans read only the density of the bone, not necessarily giving any clue as to the bone strength. Indeed, it has been argued that a reading of low bone density is not the best predictor of fracture risk (see list below).
Bones are not static or solid like bricks. They are alive just like all the organs of the body. Bones are ever-changing within the system, and pretty much in charge of this process are two kinds of special cells. First there are the osteoblasts. These are the cells responsible for depositing (laying down) new tissue in the bone). Osteoclasts do the opposite. They break down bone tissue. So it’s not hard to see that, if either of these activities are out of sync, then bone density will probably be affected. That's why it is so important to make sure that our diets contain the right kind of foods to support this process.
Everyone loses some bone density as the years advance but it’s estimated that approximately 33% of all women are potentially at risk from OP. One in every four over the age of sixty and half of those over seventy are likely to be affected. Around 100,000 fractures of hips and spines occur every year and more women die from complications following fractures than from major female cancers! Scary huh?
Osteoporosis is sometimes known as the silent disease because it may be present in the body for a long time without us noticing any symptoms. And as far as those symptoms are concerned, there may be some back pain, the odd muscle spasm or a slight curving of the spine or nothing at all until someone slips or trips. By the time thinning bones show up on an ordinary X-ray, as much as 30 percent of bone mass could already have been lost. That's why the recommended test is a bone density scan - usually done on the hip and the spine - which shows, as the name suggests, the existing density of those areas. However, bear in mind that scans read only the density of the bone, not necessarily giving any clue as to the bone strength. Indeed, it has been argued that a reading of low bone density is not the best predictor of fracture risk (see list below).
Bones are not static or solid like bricks. They are alive just like all the organs of the body. Bones are ever-changing within the system, and pretty much in charge of this process are two kinds of special cells. First there are the osteoblasts. These are the cells responsible for depositing (laying down) new tissue in the bone). Osteoclasts do the opposite. They break down bone tissue. So it’s not hard to see that, if either of these activities are out of sync, then bone density will probably be affected. That's why it is so important to make sure that our diets contain the right kind of foods to support this process.
FACTORS WHICH INCREASE RISK:
|
Family history of osteoporosis
Being above average height Being too thin Too much exercise Too little exercise A sedentary lifestyle Anorexia/bulimia Smoking Certain thyroid diseases and conditions Long term steroid medication, mood altering drugs, tranquillisers High intake of calcium-only supplements Antacids High intake of alcohol Too much coffee Excessive stress Depression Poor muscle strength Hormonal imbalances and conditions such as irregular periods Hormonal diseases such as PCOS |
Diets containing disproportionate amounts of meat, poultry, fish and dairy foods
Diets generally low in salads, fresh juices, vegetables and fruit** Low fat diets Regular low calorie dieting habits Diets high in wheat bran fibre or other foods containing phytates Diets high in refined carbohydrates (white flour/sugar) Diets that contain too little fluids, especially low water intake, and rely too heavily on fizzy drinks such as colas. Hypochlorhydria (low stomach acid) Poor digestion/absorption of nutrients Poor sleep pattern/insomnia **Certain vegetables may not be helpful if taken often or in large amounts. Spinach, whilst being high in fibre and calcium, is also loaded with a substance known as oxalic acid which can interfere with calcium absorption. And although there is no definitive proof, it appears from empirical evidence that foods from the nightshade family (chilli, paprika, potatoes, bell peppers, aubergine [eggplant] and tomatoes) may affect calcium balance. |
|
The good news amongst all this gloom is that it’s never too late to make a difference. Whatever our age, the time to take action is NOW whether you are looking for treatment options or, ideally, prevention. While there’s no definite cure for OP and no treatment that’s completely effective, there are a number of options well worth considering.
1. Anyone suffering from unexplained joint or back pain, thinks that they may have lost height, notices curvature of the spine, has a family history of osteoporosis or hormonal disorders, has experienced an early menopause or who has undergone a full hysterectomy, should definitely take advice. 2. Your doctor may recommend a full health check, blood work and a bone scan so that you can either be reassured or at least know what you’re dealing with. But don't get into a panic if your results are less than perfect. 3. If the situation seems to be serious or medication is recommended, I'd ask for more than one opinion. Unfortunately, the medical options currently on offer – i.e. hormone replacement therapy (HRT), bisphosphonates and selective oestrogen receptor modulators (SERMs) - all have risks attached so, if any are suggested to you, I would urge you to do your research before making any decisions as to pharmaceutical drugs. 4. Improvements to diet and lifestyle should be a top priority. There are lots of tips on these pages to help you along. Positive pH What several studies do show (and here's the encouraging news) is that upping our intake of fruits and vegetables can potentially improve the density of our bones by a staggering 80+%. And for a very good reason. Although it sounds unlikely - let's face it, we are so used to being brainwashed by the mantra that nothing but calcium-rich foods will save us - the truth is that, to maintain long term bone health, it's vital to maintain something called the blood pH (the scale we use to measure the alkalinity or acidity of a solution) at a level that is slightly alkaline. Don't be put off by the tecky chemistry stuff. Proteins and carbs are acid-forming because they leave an acid residue in the system after digestion. Vegetable, salads and fruits do the opposite, having an alkalising effect on the blood. It's important to know that when blood pH is low (in other words, when blood is too acidic) it causes calcium (and magnesium) to be pulled from the bones. Too much acidity in the blood can also hamper the actual absorption of calcium, magnesium and Vitamin D so getting the pH levels right is now seen to be one major key to reducing fracture risk. And here is where the right kind of diet can be one of the most powerful tools in the fight against OP. HIGHLY RECOMMENDED Have a look at this really excellent website. It has some of the best help around for anyone worried about osteopenia and/or osteoporosis www.algaecal.com |
The case for calcium
The main mineral associated with bones is calcium. No surprise there. Ninety-nine percent of the skeleton is made from it (in the form of salts of calcium phosphate). And it is an important mineral in the diet. Large amounts of calcium are lost naturally each day through the urine and must be replaced. If you’re menopausal or post-menopausal, most authorities recommend that you should be having 1200mg of calcium daily. Unfortunately, most people have no idea how much calcium they’re getting from their diet but it isn’t difficult to check. If you need to know, remember that most packaged foods will show their calcium content. And the Internet is full of nutrient tables. I have also recommended some useful weblinks at the foot of this article where you can check calcium quantities in foodstuffs. However, although calcium is much vaunted as THE mineral for osteoporosis, this doesn't mean that all you have to do is take a calcium supplement. There are several reasons why this is not a good idea: 1. First of all, not all types of calcium supplements are helpful. See below for what's best to take and what's best to avoid. I've spoken with several experts who believe that plain calcium carbonate (the one most often sold over the counter and still prescribed by many medics) is best avoided because of its poor bio-availability to the body. There are much better types available. 2. Second of all, calcium doesn't work in isolation. Other nutrients are vital, such as Vitamin D3, Vitamin K2, the little-known minerals called Boron and Silica. And Magnesium, often overlooked but so very important. That's why supplements that contain just calcium and nothing else probably won't work well. If your body lacks magnesium, this can seriously affect the mineral balance of the body. Some health experts believe that, in the absence of magnesium and other supporting nutrients, calcium can be 'pulled’ from the bones, which then can get either caught up in areas of soft tissue, including the arteries; or excreted from the body which means that instead of helping you, it's gone down the toilet. Hence the old phrase 'bedpan bullets' used to describe tablets that don't get absorbed. Crystals of calcium can also collect in connective tissue causing pain and disability. And when it finds its way into the arteries, it can create just as many problems as other heart-risk debris. So, although calcium is an essential mineral, it can also be 'mishandled' internally by the body and end up in places where it shouldn't be, especially when there aren't enough supporting nutrients in the diet. Certainly, when it comes to OP, an increasing body of research suggests that magnesium is as important as calcium in preventing and treating the disease. But there are also new and exciting supplements on the market which supply calcium from algae (seaweed), providing truly absorbable calcium which, studies appear to show, can really help bone health. 3. Perhaps most importantly, around two thirds of the studies that look into calcium and osteoporosis show that supplementing calcium and/or milk had little effect on the risk of fractures. Even high calcium intake during childhood is, it seems, no guarantee against OP in later life. What's especially interesting to note is that in countries where people rarely use calcium supplements and/or don't drink milk anyway, the number of fractures is at least 50 per cent less than in countries where milk and calcium are heavily promoted and consumed. So whilst the right type of calcium from food sources is essential, it's just as important to choose a well-absorbed type of calcium supplement and all those really important supporting nutrients. |
WHAT ELSE CAN YOU DO
TO HELP YOURSELF:
Eat more alkaline-forming foods (fruits and vegetables) and less acid-forming foods (proteins and starches). Why do you need to do this? Well, as we've seen above, a diet that contains too much meat, fish, poultry, cow's milk and refined carbohydrates (especially if it's low in veggies) ups the acidity of the blood whereas a balanced intake of protein with plenty of vegetables, salads, fresh juices and fruit (even though it may not seem to be so rich in calcium) does the opposite, helping to lay essential minerals into bone rather than leaching them out. It's been estimated that we need only a couple of servings of fruit, veg or salad to neutralize the acidity of one helping of starchy grains and only 3 servings of vegetable, fruit or salad stuff to balance the acidity we produce in the eating of just 1 serving of animal protein. The proven benefits of balancing the diet by taking in more alkaline-forming foods could also be why studies show the Mediterranean diet to be beneficial for bone health.
I have long been an advocate of this type of diet and have written about it in many press and magazine articles and in several books. More information on acid and alkaline-forming foods can be found on pages 420-437 of my book The Complete Book of Food Combining.
I have long been an advocate of this type of diet and have written about it in many press and magazine articles and in several books. More information on acid and alkaline-forming foods can be found on pages 420-437 of my book The Complete Book of Food Combining.
|
PAY SPECIAL ATTENTION TO YOUR DIET: Milk: It's a common misconception that cow's milk is the only worthwhile source of calcium for humans. Indeed, milk is often touted as the best source of this mineral which is true if you happen to be a calf. But even though it's fine to include milk in the diet, cow’s milk doesn't suit everyone. It isn't possible to absorb calcium from milk unless it’s digested properly and the fact is that many people don't fully digest milk products. Sometimes they can't digest the protein or the natural sugar in milk, called lactose, or find they have constant problems with mucus (a common side-effect of drinking milk). Indeed, it's estimated that around two-thirds of the world population is unable to properly digest cow's milk and for the vast majority, processed pasteurised milk has never been a natural part of the diet anyway. The good news is that there are lots of other dairy and non-dairy foods that provide valuable amounts of this important mineral. It's worth knowing that, unless you have an allergy to dairy products, the calcium from natural yoghurt and from good quality cheeses is likely to be better absorbed by the body than the calcium from milk. This is not only because the often indigestible lactose found in milk is broken down during the manufacturing process but also because yoghurt and good cheeses contain probiotic bacteria which help digestion and absorption of this mineral. If you include as many things as possible from the food lists in this feature, you should be taking on board not only calcium but also the B complex, vitamin D, vitamin C, manganese, boron, zinc and magnesium, all of which work with calcium to support bone health. EFAs: Essential fatty acids known as Omega 6 - found in nuts, seeds, cold-pressed oils and in evening primrose oil, starflower and GLA supplements, are known to improve calcium balance and calcium levels in bone. And the one we know so well as Omega 3 (which comes from fish oils and is found in flaxseed and walnuts) is also a calcium assisting nutrient. Calcium supplements: If you have any doubts about your intake of OP-protective nutrients, it could be a wise move to consider supplements – but do please take care. For example, many include the cheap and poorly absorbed calcium carbonate. Whilst this particular type of calcium has been shown to increase bone density, the problem with it is that it reduces stomach acid (which is why it is also used in some antacid preparations). Lowered gastric acid equals a higher alkaline environment in the stomach which, in turn, reduces the absorption of calcium. Formulae that contain calcium citrate, gluconate, aspartaate or ascorbate are likely to be far more efficiently absorbed. Other nutrients are vital too: Apart from the need for a diet high in alkaline-forming foods which we talked about above, the mineral magnesium is just as important as calcium. Magnesium is an absolutely essential ingredient when it comes to making bone and yet, sadly, low magnesium levels are all too common in the diets of so-called developed countries. Indeed, throughout my career in clinical practice, I have found so many incidences of magnesium deficiency that I sometimes wonder if it wouldn't be a good idea to supplement this mineral routinely. If your diet is low in magnesium but high in calcium (maybe you're taking additional calcium tablets or consuming a high intake of dairy foods because you think it is good for your bones?), you could actually be increasing the likelihood of brittle bone disease by disturbing the balance of nutrients. If you're unsure about your magnesium status, talk to your health professional about getting tested. Get them to look at red cell magnesium, a far more accurate way of assessing levels of this mineral than just assessing regular levels in the blood. Boron: While getting enough calcium in the diet is not that difficult, making sure that it’s properly absorbed is a whole other issue. I have studied several reports that have found losses of calcium via the urine of as much as 50-70%! One of several things that can make a difference to the way calcium behaves in the body, improving absorption and reducing the amount excreted is a little known trace mineral called boron. In people with low boron levels, more calcium is excreted. Boron, a little known mineral that's needed in only tiny quantities, helps to hang on to calcium and keep it in the bones. And it assists an oestrogenic hormone known as 17-beta estradiol which itself is vital for a healthy skeletal structure. And while it is well known that boron supplements increase bone strength, other studies show that low boron is associated with an increase risk of arthritis. In areas of the world with higher boron in the soil, there is correspondingly far less arthritis. Away from the subject of bones just for a moment, I also came across some interesting research which linked boron to cognitive function (perception, understanding, ability to process thought, to reason and make judgments. Those with low levels of boron had poorer manual dexterity and hand-to-eye co-ordination, worse attention span and greater difficulty with both short and long-term memory. Boron comes from things grown in the soil. Some experts say that we should be able to get the tiny quantities of boron needed for good health from our diet (it is found in trace amounts in nuts, vegetables and fruits) but others are convinced that the vast majority of the population are deficient in boron (a) because we don't consume enough fresh produce and (b) because it is no longer abundant in these foods anyway. The problem is that you need to eat at least 2 servings of vegetables or salad and 2 pieces of fruit each day to get enough of this mineral and that will only apply if the foods you are consuming are grown in boron-rich soil. If you are looking to take a mineral supplement of calcium and magnesium, make sure it has boron, too, or take boron in a separate supplement. Silica, also required only in small amounts, is another trace element essential to encourage bone strength. |
A Mediterranean diet rich in olive oil and fresh fruit and vegetables has been shown to benefit the bones. A GOOD HABIT TO GET INTO IS FOR EACH MEAL TO HAVE EITHER ONE THIRD PROTEIN WITH TWO THIRDS VEGETABLES (OR SALAD) OR GO FOR ONE THIRD STARCHY FOODS WITH, AGAIN, TWO THIRDS VEG OR SALAD. AND TO EAT LOTS OF FRUIT BETWEEN MEALS. Look at this wonderful selection of deliciously healthy foods. If you’re including all or most of the things in these lists, you should be getting plenty of protective nutrients as well as helping your blood to maintain the right levels of slightly alkaline pH. Just remember that when you eat protein foods such as fish, meat or dairy and starches like pasta, oats, rice or other grain cereals, make sure the meal is biased towards fresh vegetables, salads, fruit and fresh juices. General list of great 'bone' foods: Fruits and vegetables, for example apples, bananas, green salads, green and root vegetables – especially the stalks. Also good are seeds, sprouted beans and sprouted seeds, almonds, Brazil nuts, dried figs, ditto apricots, fresh root ginger, fresh herbs, garlic and lemons. Good proteins sources include pulses (legumes), organic soya products - such as soya milk, soya beans and tofu, fresh oily fish – especially herring, mackerel, salmon, tuna and trout. Also think about: canned salmon, canned sardines, brown rice, rye crackers, oat cakes, oat cereals, yoghurt, buttermilk and good quality naturally produced cheeses. Great news: A glass of wine three or four times a week is said to help because the alcohol has certain bone-protecting qualities. Excess alcohol has the opposite effect! Calcium: It's easy to get the wrong idea that the only real source of dietary calcium is milk. Not so! Beneficial calcium turns up in all kinds of other foods, albeit in smaller amounts yet entirely bio-available (absorbed and assimilated by the body). Specifically, the following foods are worthwhile sources of absorbable calcium. Blackstrap molasses, brown rice, canned sardines, canned pilchards and canned salmon, home-made stock (made with vegetables, including stalks and scraps, organic meat bones and/or poultry carcass), carob flour, dried fruits, fortified soya milk, nuts (especially almonds, Brazil's and unsalted cashew nuts), oats, pulses, buttermilk, yoghurt, cheese (try goat or sheep's cheese rather than those made from cow's milk), fresh herbs, sea vegetables such as hizike, wakame and nori, sesame seeds and tahini, sunflower seeds and tofu. Magnesium: Green leafy vegetables, the darker green the better, are one of the best sources of magnesium. So, too, are wholegrains, nuts (especially almonds, Brazils and unsalted cashews), pulses (legumes), soya milk, soya beans, tofu and foods made with soya flour. Bananas, figs, avocado pear, apricots, lemons, apples, garlic and ginger root contain small but worthwhile amounts of this important mineral. Foods to avoid: Cut right down on beef and pork and steer clear of deep fried and fatty foods, wheat bran fibre, salt, fizzy drinks such as cola (diet and zero are just as bad), sweet fruit cordials and root beer. All these things have negative effects on your bone minerals, being acid-forming to the blood even though they may not seem to be acidic at the time you are consuming them. Sugar is especially heinous when it comes to calcium loss from the bones. Vitamin A works with Vitamin D, calcium and magnesium to encourage strong bones. You can find the vegetable source of this vitamin, known as beta carotene, not just in carrots but also in almost any food that is orange, yellow or dark green; for example, dark leafy green vegetables such as collards, red leaf lettuce, spinach (eat in small amounts only), chard, and kale, also in cantaloup melon, yellow peppers and butternut squash. Vitamin C isn't just for colds, it's for bones too. That's because it's needed to repair collagen in bone and in skin. Although I believe it is unwise to take the cheaper type of vitamin C sold as plain ascorbic acid (such as the over-the-counter version which fizzes in water), I would certainly advocate taking 2 grams a day of a top quality buffered Vitamin C Complex such as those produced by Solgar, Viridian-Nutrition, Bionutri and Biocare. Vitamin D known as D3 (see more below) and another called Vitamin K2, are both really important bone nutrients.
XYL0TENE
Xylotene contains sweet-tasting 'nutritional' sugars xylitol and D-xylose, known as glyconutrients (quite different from the type of sugar that you put into tea or coffee). Both are helpful to bone health:
I think it's really worth taking the time to read more about Xylotene on the Sweet Cures website: https://www.sweet-cures.com/xylotene.htm |
VITAMIN D
Researchers have already shown Vitamin D it to be incredibly important in the prevention and treatment of osteoporosis. And it may be significant in reducing the risk of diabetes, high blood pressure, fibromyalgia, muscle pain and multiple sclerosis. Research published in the British Medical Journal found that high blood levels of vitamin D were associated with a lower risk of colon cancer. Deficiencies have also been associated with other forms of cancer and, in older adults, with both dementia and heart disease. If you have a digestive condition such as Crohn's disease, coeliac disease, or leaky gut syndrome, or simply don't digest well, there's a possibility that you're not absorbing enough vitamin D. Age also plays a role here. As we grow older, our bodies are less capable of converting vitamin D to its active form in the body. It's also the case that people who are considerably overweight often have reduced levels of this vital nutrient. For people who don't go out in the sun very much at all, are in a risk category for osteoporosis or are vegan, and for those who live in northern areas where there is little sun, deficiencies are more common. The old advice that we should only take it in tiny amounts because of a potential risk of liver toxicity was, for decades, apparently based on nothing more than assumption. Although we call it a vitamin, this nutrient is actually a hormone and we now know it can be taken in larger quantities. I use 1000 iu per day. My sister-in-law - a nurse, who lives where Ice Road Truckers rule and daylight is in desperately short supply – tells me that prescriptions of 5000 iu daily are routine. However, do please check with your GP or nutrition adviser before taking this nutrient as there are a few conditions where larger doses are not recommended and could be dangerous. Natural food sources of D include cheese, liver, eggs, fish, especially salmon and tuna, fish oils and milk.
|
Experience in clinical practice suggests that the combination of good quality magnesium with Vitamin D can help to ease chronic pain and tension for some people. For excellent quality magnesium and vitamin D supplements, consider Viridian-Nutrition or Biocare.
|
In pain or suffering muscle tension?
It's worth knowing that Magnesium (as magnesium malate, glycinate, orotate or taurine) and Vitamin D3 can also be supportive when it comes to pain control. |
WHAT ELSE?
Eat more vegetarian and vegan dishes.This doesn't only help the blood pH, it also helps the purse. Vegetable based meals cost far less to produce and to buy than animal protein. You don't need to go completely vegetarian or vegan (unless that is your personal choice) but upping the veggie intake and going for non-meat dishes is not only nutritious but can be just as filling and sustaining. Better for your bodyweight, your bones and your cardiovascular health too.
Do whatever you can to deal with stress and mood changes. Both excessive stress and depression can increase your risk of OP. That’s because the stress hormone called cortisol – which tends to be over-produced in people who suffer from ongoing stress or clinical depression – has a direct effect on bone density. Cortisol has been found to decrease osteoblasts (remember these are cells which are active in making new bone tissue). When there aren’t enough osteoblasts to do this job, more bone matrix is broken down (lost from the skeleton) than is made (deposited in the skeleton) which, overtime, inevitably results in greater risk of porous bones. A similarly negative effect is known to be caused by corticosteroid medications. And it's worth repeating what I said elsewhere in these pages: Persistent depression that won't resolve, especially if it's associated with chronic fatigue, can be a sign of low magnesium levels, so if that sounds like you, then why not get yourself tested?
Get Moving: Whatever treatment an OP sufferer chooses, regular load bearing exercise is regarded as an essential component in improving bone strength. Both yoga and pilates are highly recommended. If fitness is a problem, remember that even simple standing or sitting exercises and stretches are better than no activity at all. Swimming, although not load-bearing, is also known to be valuable.
Manage your weight: There's little doubt that carrying extra weight puts huge strain on the joints, especially hips, knees and spine. So being overweight does your skeletal frame no favours. But although carrying excess kilos is not a great idea, going too far the other way is a REALLY BAD IDEA. Why? Well, while excess weight can be a big health risk, it's worth knowing that a bit of extra padding at the menopause may offer some protection against brittle bones. That’s because small amounts of essential oestrogen are stored in fat tissue, especially subcutaneous and abdominal fat. Being too skinny can increase the risk of osteoporosis. Whatever your weight, don't ever be tempted to yo-yo diet or to follow any kind of very low calorie regime. There are far safer and healthier ways of getting your weight to where it should be. If you're trying to lose weight and have been on lots of weight loss diets but got nowhere or put it all back on, have a look at my guide to HEALTHY WEIGHT LOSS.
Get out in the sunshine: Avoid excessive sun but don’t forget that 10-15 minutes a day of sensible sun exposure helps to activate Vitamin D which is not only needed for calcium absorption but, as mentioned already, also has many other health benefits. Encouragingly, there is new research to show that higher doses (1000-2000 iu daily) of vitamin D not only minimises risk of hip fractures in post-menopausal women but may also reduce the risk of falls in the elderly. I would certainly advocate taking at least 1000 iu of vitamin D each day alongside a good calcium/magnesium supplement. But do take professional medical and nutritional advice on this point. Worth emphasising: People who are unable to tolerate any sun exposure or who wear long robes or head coverings, or are in a risk category for osteoporosis, or who live in northern areas where there is little sun, can be at greater risk of Vitamin D deficiency and may be advised to look to diet to increase their Vitamin D intake.
Consider the damage caused by smoking: Try to avoid cigarette smoke, yours or other peoples’. Research shows a very definite link between smoking and decreased bone mineral density.
Enjoy alcohol but . . . stick to a maximum of a glass of wine per day and forget about beer, lager and spirits.
I know I've said this already but do make every effort to avoid foods that are based on white flour or are high in sugar, such as white bread, cakes, biscuits, sugary snacks etc.
Instead of red meat, get your protein from pulses (peas, beans and lentils), soya protein and lesser amounts of lean poultry and fish.
Watch that tea and coffee intake. If you're a fan of coffee and black tea, try to cut back on these and introduce more herbal teas, fresh fruit and vegetable juices and plenty of water. Caffeine, in particular, increases the rate at which calcium is lost from the body via the urine.
Take a good quality supplement. As a boost to a healthy diet, I would say go for a good multi combination designed especially for bone health that contains calcium, magnesium, boron, silica, vitamin D3 and vitamin K2. Never take calcium supplements in isolation or cheap priced minerals. In my own clinical experience and that of other colleagues, low cost supplements very often contain low quality and/or poorly absorbed ingredients, are not properly balanced and have too few (or none at all of the necessary) supporting ingredients. A good rule is to buy the absolute best that you can afford. It's better to take a quality product every other day or even every other month than a cheap one all the time. Have a look at quality supplements produced by companies such as Viridian Nutrition, Biocare, or Solgar). The Natural Dispensary www.naturaldispensary.co.uk and Sunshine Health Shop www.sunshinehealthshop.co.uk in the UK have a wide range of excellent food supplements and despatch to a long list of overseas countries.
Take probiotics. Healthy gut bugs play an important role in mineral absorption. Read more on this by clicking this link. And then this link, too.
Check out the diet section above and also have a look at the healthy eating advice on other pages of this website including HEALTHY BYTES and COLOUR YOUR WAY TO A HEALTHIER DIET.
Do whatever you can to deal with stress and mood changes. Both excessive stress and depression can increase your risk of OP. That’s because the stress hormone called cortisol – which tends to be over-produced in people who suffer from ongoing stress or clinical depression – has a direct effect on bone density. Cortisol has been found to decrease osteoblasts (remember these are cells which are active in making new bone tissue). When there aren’t enough osteoblasts to do this job, more bone matrix is broken down (lost from the skeleton) than is made (deposited in the skeleton) which, overtime, inevitably results in greater risk of porous bones. A similarly negative effect is known to be caused by corticosteroid medications. And it's worth repeating what I said elsewhere in these pages: Persistent depression that won't resolve, especially if it's associated with chronic fatigue, can be a sign of low magnesium levels, so if that sounds like you, then why not get yourself tested?
Get Moving: Whatever treatment an OP sufferer chooses, regular load bearing exercise is regarded as an essential component in improving bone strength. Both yoga and pilates are highly recommended. If fitness is a problem, remember that even simple standing or sitting exercises and stretches are better than no activity at all. Swimming, although not load-bearing, is also known to be valuable.
Manage your weight: There's little doubt that carrying extra weight puts huge strain on the joints, especially hips, knees and spine. So being overweight does your skeletal frame no favours. But although carrying excess kilos is not a great idea, going too far the other way is a REALLY BAD IDEA. Why? Well, while excess weight can be a big health risk, it's worth knowing that a bit of extra padding at the menopause may offer some protection against brittle bones. That’s because small amounts of essential oestrogen are stored in fat tissue, especially subcutaneous and abdominal fat. Being too skinny can increase the risk of osteoporosis. Whatever your weight, don't ever be tempted to yo-yo diet or to follow any kind of very low calorie regime. There are far safer and healthier ways of getting your weight to where it should be. If you're trying to lose weight and have been on lots of weight loss diets but got nowhere or put it all back on, have a look at my guide to HEALTHY WEIGHT LOSS.
Get out in the sunshine: Avoid excessive sun but don’t forget that 10-15 minutes a day of sensible sun exposure helps to activate Vitamin D which is not only needed for calcium absorption but, as mentioned already, also has many other health benefits. Encouragingly, there is new research to show that higher doses (1000-2000 iu daily) of vitamin D not only minimises risk of hip fractures in post-menopausal women but may also reduce the risk of falls in the elderly. I would certainly advocate taking at least 1000 iu of vitamin D each day alongside a good calcium/magnesium supplement. But do take professional medical and nutritional advice on this point. Worth emphasising: People who are unable to tolerate any sun exposure or who wear long robes or head coverings, or are in a risk category for osteoporosis, or who live in northern areas where there is little sun, can be at greater risk of Vitamin D deficiency and may be advised to look to diet to increase their Vitamin D intake.
Consider the damage caused by smoking: Try to avoid cigarette smoke, yours or other peoples’. Research shows a very definite link between smoking and decreased bone mineral density.
Enjoy alcohol but . . . stick to a maximum of a glass of wine per day and forget about beer, lager and spirits.
I know I've said this already but do make every effort to avoid foods that are based on white flour or are high in sugar, such as white bread, cakes, biscuits, sugary snacks etc.
Instead of red meat, get your protein from pulses (peas, beans and lentils), soya protein and lesser amounts of lean poultry and fish.
Watch that tea and coffee intake. If you're a fan of coffee and black tea, try to cut back on these and introduce more herbal teas, fresh fruit and vegetable juices and plenty of water. Caffeine, in particular, increases the rate at which calcium is lost from the body via the urine.
Take a good quality supplement. As a boost to a healthy diet, I would say go for a good multi combination designed especially for bone health that contains calcium, magnesium, boron, silica, vitamin D3 and vitamin K2. Never take calcium supplements in isolation or cheap priced minerals. In my own clinical experience and that of other colleagues, low cost supplements very often contain low quality and/or poorly absorbed ingredients, are not properly balanced and have too few (or none at all of the necessary) supporting ingredients. A good rule is to buy the absolute best that you can afford. It's better to take a quality product every other day or even every other month than a cheap one all the time. Have a look at quality supplements produced by companies such as Viridian Nutrition, Biocare, or Solgar). The Natural Dispensary www.naturaldispensary.co.uk and Sunshine Health Shop www.sunshinehealthshop.co.uk in the UK have a wide range of excellent food supplements and despatch to a long list of overseas countries.
Take probiotics. Healthy gut bugs play an important role in mineral absorption. Read more on this by clicking this link. And then this link, too.
Check out the diet section above and also have a look at the healthy eating advice on other pages of this website including HEALTHY BYTES and COLOUR YOUR WAY TO A HEALTHIER DIET.
For more information, try these websites:
Also read: Anne Marie Colbin
Just as I was putting the finishing touches to this article, I suddenly remembered a fantastic book that I bought back in the late 90s that I think would be helpful to anyone wanting to learn more about keeping bones healthy. Not even sure it's still in print but second hand copies are around. It's called Food and Our Bones by the genius nutrition doctor Anne Marie Colbin. It is still an entirely relevant, beautifully written and extremely informative book.
Last time I looked, Food and Our Bones was available from www.amazon.co.uk and www.amazon.com
To read about Dr Colbin and her work go to: www.foodandhealing.com
AND MORE . . .
|
Sites talking about calcium and calcium rich foods:
http://www.iofbonehealth.org/patients-public/about-osteoporosis/prevention/nutrition/calcium-rich-foods.html http://www.osteoporosisadvice.com/calcium-levels-foods.php http://pediatrics.about.com/od/calcium/a/06_calcium_food.htm |
Sites which discuss about the role of other supplements such as magnesium, strontium and algae sourced calcium in osteoporosis:
https://www.consumerhealthdigest.com/bone-support-reviews/algaecal-plus.html https://www.algaecal.com/osteoporosis-treatment/ https://www.algaecal.com/where-to-buy-algaecal-plus/ http://www.mgwater.com/gaosteo.shtml http://www.mgwater.com/index.shtml http://www.healthcentral.com/osteoporosis/c/3414/11813/magnesium |
Kathryn's views are completely independent. She is not employed by any pharmaceutical company, supplement supplier or food producer nor is she persuaded in any way, financially or otherwise, to recommend particular products or services.